Cardiology and Stroke Research
Health Tips
Medical Conditions
Medical-Innovation
Resting heart rate and stroke risk
Stroke Research
anticoagulation, asundexian, atrial fibrillation, breakthrough stroke, cardiac amyloidosis, cardiology research, carotid atherosclerosis, esoc 2026, factor xia inhibitor, healthy lifestyle, ischemic stroke, oceanic-stroke trial, resting heart rate stroke risk, stroke prevention, stroke severity, wellness
Carolyn Stinnett
0 Comments
Powerful 5 Cardiology and Stroke Research Breakthroughs for Better Heart Health
Cardiology and Stroke Research and Stroke Research: What the Latest Studies Mean for You 5
Roughly 795,000 people in the U.S. have a stroke each year, according to CDC estimates. About one in five survivors will have another within five years. This spring, the European Stroke Organisation Conference (ESOC) 2026 presented several studies that could shift how clinicians approach stroke prevention, heart rate monitoring, and the frustrating problem of strokes that happen despite blood thinners.
My strong feeling after reviewing these results: we’ve been too passive. Too willing to shrug at unexplained treatment failures and too slow to use cheap, available data like resting heart rate. Some of the ESOC findings back that up.
Factor XIa inhibitors and stroke severity
The biggest news came from new analyses of the OCEANIC-STROKE trial, a Phase III study of over 12,000 patients testing asundexian, an oral Factor XIa inhibitor made by Bayer. Factor XIa is a clotting protein, but it’s more involved in the harmful clot formation that causes strokes than in the everyday clotting that stops a cut from bleeding. That distinction is the whole ballgame. Traditional blood thinners reduce dangerous clots but increase bleeding. Factor XIa inhibitors are designed to break that tradeoff.
Latest Cardiology and Stroke Research on Prevention
The primary results, published in the New England Journal of Medicine, showed asundexian reduced ischemic stroke without increasing major bleeding. The new ESOC data went deeper. Among patients who still had a stroke during the trial, those on asundexian had less severe events. Only 22.9% of strokes in the asundexian group scored 8 or higher on the NIH Stroke Scale (a standard severity measure), compared to 30.3% in the placebo group. Disabling strokes were less common too: 2.1% versus 3.0%.
Fewer patients on asundexian needed emergency clot-retrieval procedures. Fewer had fatal strokes, though that particular difference did not reach statistical significance.
Factor XIa inhibitors are not yet approved for stroke prevention. But the trajectory of the data is hard to ignore.
Resting heart rate and stroke risk
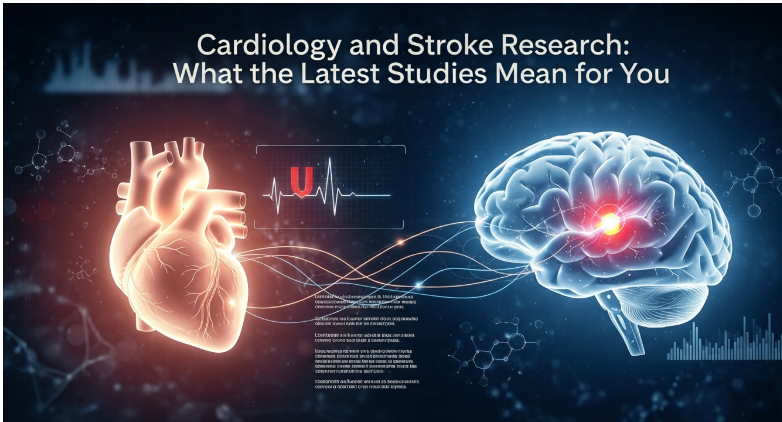
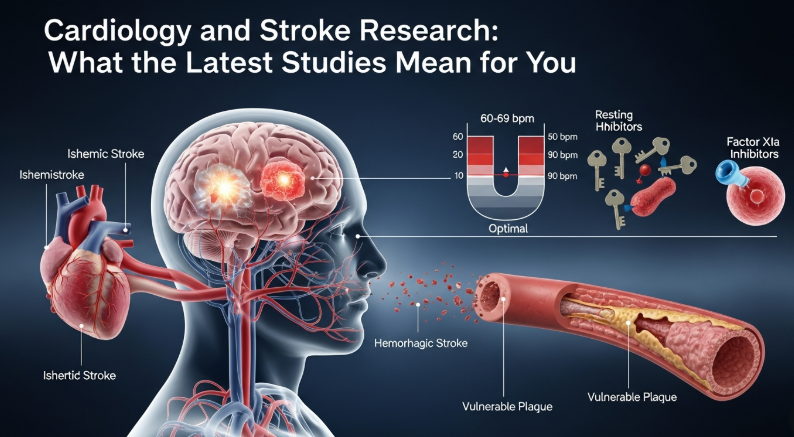
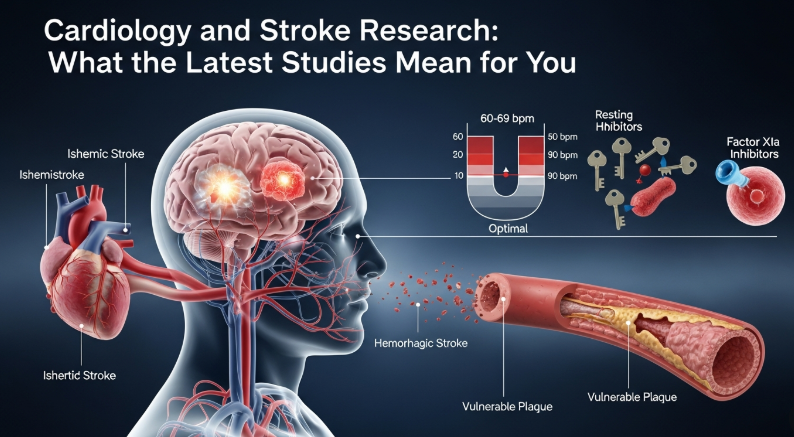
Another ESOC 2026 study, drawing from nearly 460,000 UK Biobank participants followed for an average of 14 years, found a U-shaped relationship between resting heart rate and stroke risk. The lowest-risk range was 60 to 69 beats per minute. Below 50 bpm, risk was about 25% higher. At 90 bpm or above, it climbed to roughly 45% higher.
The low-end finding will surprise people. We associate a slow heart rate with fitness. Often correctly. But very low rates may reduce blood flow to the brain by stretching the gap between heartbeats too long. On the high end, elevated rates may reflect chronic stress on vessel walls, contributing to both ischemic and hemorrhagic stroke.
One wrinkle: the U-shaped pattern held up in people without atrial fibrillation but vanished in those who had it. Atrial fibrillation raises stroke risk by about fivefold, which swamps the heart rate signal.
Professor Alastair Webb, one of the study’s senior authors at Imperial College London, said resting heart rate is a simple, widely available measure that “deserves greater attention in cardiovascular risk assessment.” He is right, and it’s kind of baffling that we don’t pay more attention. It’s free. Takes ten seconds. And once arrhythmia has been ruled out, most clinicians never think about it again.
Breakthrough strokes on blood thinners
Recent Cardiology and Stroke Research continues to reshape preventive healthcare strategies worldwide.
About 20% of strokes in patients with atrial fibrillation happen despite anticoagulation. These “breakthrough strokes” carry a recurrence risk of 5% to 9% per year, and there is no great secondary prevention strategy for them. Switching anticoagulants doesn’t clearly help. Adding aspirin can cause harm.
A large German registry study called RASUNOA-Prime presented findings that may explain part of the puzzle. Among nearly 1,500 patients with AF and acute ischemic stroke who had CT angiography, 81% had some form of carotid atherosclerosis. Seventeen percent had significant narrowing or blockage.
Here’s the key finding: in patients on direct oral anticoagulants who had a stroke anyway, the odds of finding a vulnerable carotid plaque on the same side as the brain injury were about four times higher than on the opposite side. These aren’t the dramatic vessel-blocking plaques from a textbook diagram. They’re softer, more unstable lesions, the kind that can rupture and send debris into the brain without ever producing a significant blockage on their own.
This matters. It suggests that for some patients, breakthrough strokes aren’t a failure of anticoagulation against heart-origin clots. They’re a different problem, one that might call for more aggressive lipid management or targeted imaging surveillance. If you’re on blood thinners for AF and still had a stroke, the question of whether anyone has imaged your carotid arteries is a reasonable one to raise with your doctor.
Experts in Cardiology and Stroke Research are now focusing on carotid plaque imaging and anticoagulant safety.
Cardiac amyloidosis and stroke
Many physicians believe Cardiology and Stroke Research will soon focus more on biological risk prediction. and Future developments in Cardiology and Stroke Research may improve survival rates and long-term recovery outcomes.
A Danish nationwide cohort study, published in *JACC: Heart Failure*, found that cardiac amyloidosis was not associated with a higher risk of stroke or TIA compared to matched controls. It was linked to more bleeding-related hospitalizations. A useful distinction. Not every cardiac condition raises stroke risk the same way, and clinicians managing amyloidosis patients shouldn’t assume it does.
What to do with this
Cardiology and Stroke Research reveals 7 powerful breakthroughs in stroke prevention, anticoagulants, carotid plaque detection, and heart health treatment strategies.
None of these findings mean you should change your medications on your own. But a few things are worth raising at your next appointment.
If you’ve had a stroke or TIA, ask about newer prevention strategies. Factor XIa inhibitors aren’t approved for this use yet, but the data are moving fast. If your resting heart rate is consistently below 50 or above 90 and you don’t have atrial fibrillation, bring it up. If you’re on anticoagulants for AF and had a stroke anyway, ask whether your carotid arteries have been checked. Plaque buildup may be a factor that blood thinners alone won’t address. And do not stop or adjust anticoagulants without talking to your doctor. The bleeding risks are real.
The RASUNOA-Prime data, to me, are the most thought-provoking results of the bunch. We still don’t know whether routine carotid imaging in AF patients on anticoagulants would change outcomes, or whether it would just generate anxiety and procedures. That study hasn’t been done yet.
*This article is for informational purposes only and does not constitute medical advice. Always consult your own healthcare provider before making changes to your treatment.*












Post Comment